Given its broad scope, we are always interested in emerging frameworks that can help us better measure patient experience, and allow organizations to continually learn, grow, and implement changes both small and large to improve patients’ experiences.
In their paper “Routine measure of patient experience,” Tim Benson and Alex Benson present a compelling framework that healthcare organizations can use to assess the effectiveness and quality of their patient experience. This framework incorporates three different but complementary dimensions to explore when gathering patient perspectives:
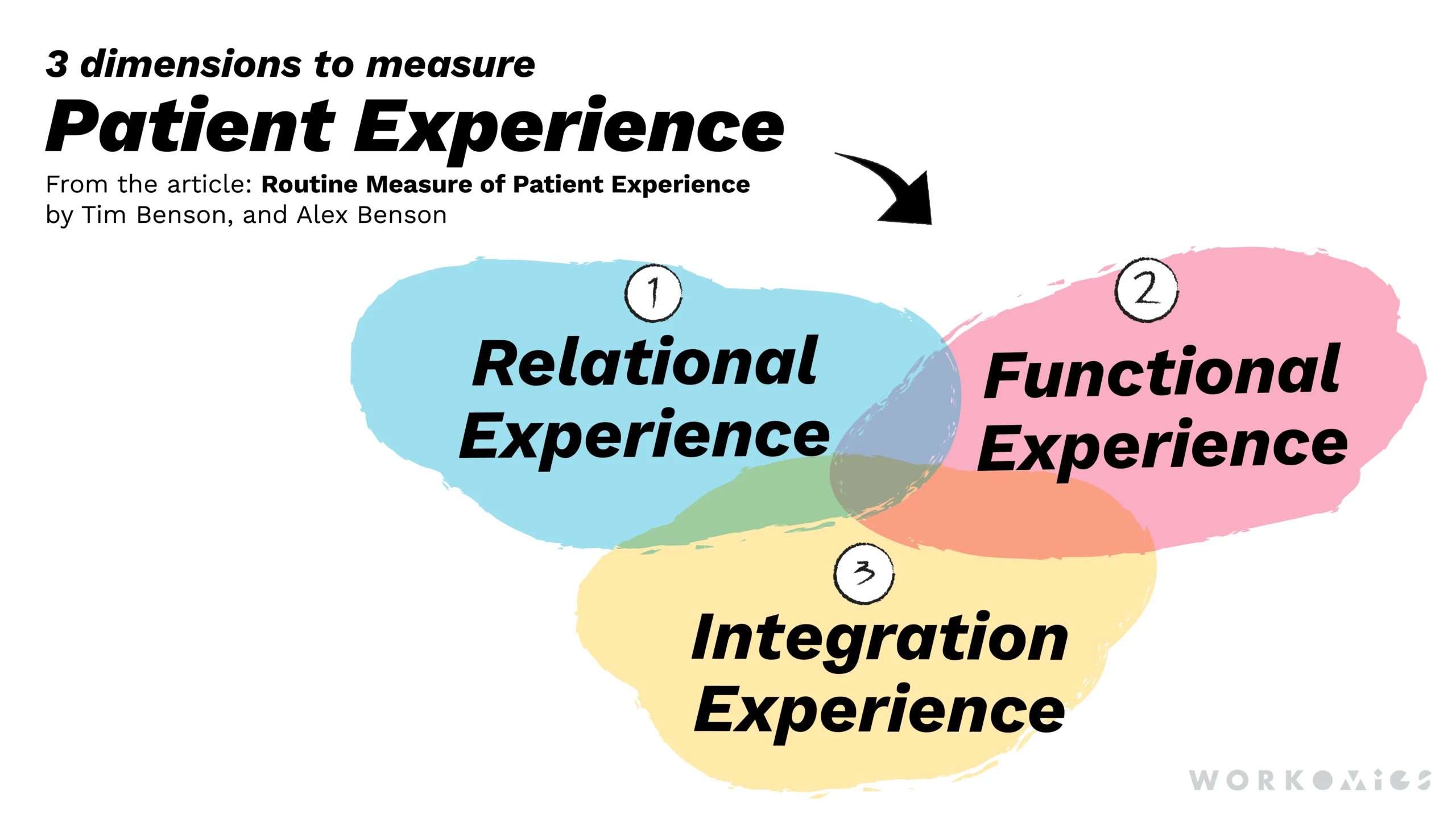
Relational experience
This dimension focuses on the interaction between clinicians and patients. It is the primary focus of most efforts to improve patient engagement and patient-centred care. This is further subdivided into the following subcategories:
- Compassion covers how individuals are treated directly, including empathy, politeness, respect, and privacy.
- Communication includes two-way interaction between patients and clinicians, such as engagement, information sharing, education, consent, shared decision-making, and empowerment.
- Timeliness covers all types of delay, waiting times, access, cancellations, and responsiveness.
- Reliability covers how well the unit is managed, including safety, dependability, efficiency and availability and use of information (e.g., lab results).
Functional experience
This concerns the immediate benefits perceived by patients at the time of treatment. However, it does not cover medium and long-term benefits or patient outcomes. This is further subdivided into the following subcategories:
- Consultation includes face-to-face, video or telephone sessions with clinicians or provider staff.
- Treatment covers all types of care, therapy and medication given, prescribed or changed.
- Practical help covers arrangements made or promised, if any.
- Plan covers future plans, tests and referrals, including doing nothing.
Integration experience
This relates to the overall experience of care that crosses traditional silos. The aim here is to facilitate “whole system” improvement and enhance broader continuity. This is further subdivided into the following subcategories:
- Communication speaks to how well services communicate.
- Service knowledge is about patients’ perceptions of staff awareness of what other services do.
- Repetition is whether patients need to repeat their stories endlessly.
- Collaboration covers how well different services work together as a team.
We see this framework as a practical and scalable structure that can help organizations translate patient feedback into tangible, positive change. We particularly appreciate this approach for a few key reasons:
First, the proposed survey categories are concise, have a low reading level, and follow a common format and scoring schema. This allows surveys to be used individually or combined, enabling organizations to examine patient experience with sufficient detail to identify specific opportunities for improvement across the broader experience. More importantly, this approach prioritizes the patient voice, making it easier to routinely and frequently solicit direct patient feedback.
Second, many standard frameworks used today tend to focus solely on the patient’s experience with individual staff members, such as doctors, nurses, and admin staff. In contrast, this framework adds new measurement dimensions to help organizations understand how well their patient experience is performing across functional and integration experience dimensions as well.
Click here to dive deeper into the Routine Measure of Patient Experience.

Our other ideas worth exploring
On Journey Mapping
Moving beyond customer-centricity theatre. An in-depth breakdown of journey maps and how to use them correctly.
Why building awareness for rare disease clinical trials matters
A framework that can help us better measure patient experience, and allow organizations to continually learn, grow, and implement changes both small and large to improve patients’ experiences.
The Participation Problem: Addressing socioeconomic barriers in clinical trials
Genetics and socioeconomic factors can influence how a drug performs, and yet, a persistent gap remains between the people who need new treatments and those represented in the clinical trial data.